If your dentist suggests a root canal, there’s no need to panic — modern endodontic care is focused on relieving pain, stopping infection, and preserving as much of your natural tooth as possible. For many patients, root canal therapy keeps chewing function intact and avoids the longer timelines and additional procedures that follow removing a tooth. The aim is practical: remove diseased tissue, protect the remaining structure, and restore comfort and function.
At Chroma Dental, our team blends precise diagnostics with a patient-centered approach to make endodontic treatment straightforward and predictable. Whether you come in with sudden, intense discomfort or a tooth that’s been troubling you for months, we prioritize clear explanations, gentle techniques, and careful follow-up so you understand what to expect at every step.
Preserving a tooth whenever clinically feasible supports long-term oral health. A natural tooth maintains the surrounding bone, preserves normal chewing patterns, and helps neighboring teeth remain stable. Once a tooth is removed, nearby teeth can shift and adjacent bone can resorb over time, which may complicate future restorative work.
Root canal therapy is a conservative strategy: it removes the infected or inflamed pulp while leaving the outer tooth largely intact. Advances in canal shaping, irrigation, and sealing materials have improved predictability, so a properly treated tooth often performs well for many years. When combined with an appropriate final restoration, the treated tooth can continue to function like its healthy neighbors.
Deciding whether to save a tooth involves more than the immediate procedure. We evaluate the amount of remaining tooth structure, periodontal support, and the anticipated strength of a final restoration. Our goal is to recommend the option that gives you the best balance of durability, function, and oral health over time.

Inside each tooth, the pulp contains nerves and blood vessels that keep the tooth alive. When bacteria reach the pulp chamber through deep decay, a crack, or an injury, the tissue can become inflamed or die. That internal change can lead to pain, swelling, and in some cases a collection of pus at the root tip, which requires timely attention.
Symptoms vary from person to person. Some people have intense, throbbing pain that interrupts sleep, while others experience only occasional sensitivity to hot or cold. Occasionally a tooth shows little discomfort despite clear infection visible on a radiograph, which is why clinical exam and imaging together are important for an accurate diagnosis.
When pulp damage is irreversible, root canal treatment removes the diseased tissue while keeping the tooth’s outer form. If enough tooth substance and bone support remain, the tooth can be restored and protected for long-term use. Early professional assessment preserves treatment options and tends to produce simpler, more predictable results.
Although toothaches don’t always mean you need a root canal, the following signs often point to pulp involvement:
Pain that persists or increases over time, especially pain that disturbs sleep or daily activities, frequently indicates internal inflammation or infection and should be evaluated promptly.
If hot or cold stimuli trigger sensitivity that lingers long after the stimulus is gone, the nerve tissue may be compromised and warrants professional assessment.
Pain on biting or feeling tenderness when pressure is applied can signal that the tooth’s internal structures or surrounding tissues are affected.
A tooth that darkens after trauma or over time can indicate loss of vitality; discoloration is a visible cue that the pulp may be damaged.
Even small fractures can provide a pathway for bacteria to reach the pulp. Any structural damage should be inspected to determine the extent of internal involvement.
An area of gum swelling, a persistent pimple-like bump, or intermittent drainage are signs that an infection may have reached the root tip or surrounding bone and need attention.
Infection that affects supporting bone can lead to mobility; addressing the source of infection early often helps protect the tooth’s long-term stability.
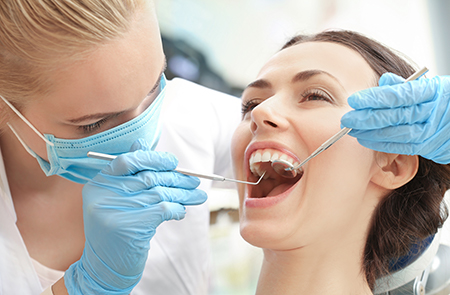
Waiting to address a problematic tooth can allow an infection to grow and spread, which often increases discomfort and the risk of damage to nearby teeth and bone. In some situations, a tooth that might have been treatable early on becomes unrestorable without extraction if care is delayed.
Regular dental exams and appropriate radiographs catch many issues before they become severe. Some teeth show minimal symptoms but reveal periapical changes on X-rays; catching these early preserves less invasive treatment choices and usually results in simpler procedures with better outcomes.
When we recommend root canal therapy, we explain the reasons behind the recommendation and review the expected steps, recovery, and restoration needs. Making informed decisions quickly helps limit complications and supports an efficient path back to comfort and function.
Today’s non-surgical root canal procedures are designed for precision and patient comfort. After anesthetizing the area, the clinician isolates the tooth and creates a small access point to reach the pulp chamber. Using magnification and specialized instruments, the canals are cleaned and shaped to prepare them for a sealing material.
Disinfection is central to success. Clinicians use proven irrigation solutions and techniques that greatly reduce bacteria in the canal system. Once the space is clean and dry, the canals are filled with a biocompatible material that seals the system and helps prevent reinfection. Local anesthesia is used throughout, and sedation options can be offered for patients who prefer them.
Some teeth are treated in a single visit; others require staged care if there is active infection or complex root anatomy. After endodontic therapy, most teeth are fitted with a definitive restoration — by far the most common is a crown — to restore strength and protect the treated tooth from fracture.
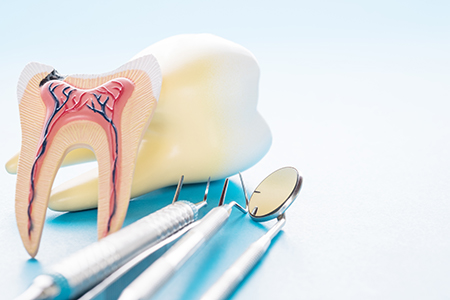
Many patients notice significant relief from the intense pain that led them to seek care. Mild soreness or tenderness around the treated tooth and gums is normal for a few days while tissues settle. Over-the-counter pain relievers typically manage this discomfort; your clinician will advise if stronger medication or antibiotics are needed.
While a temporary filling is in place, the tooth is more susceptible to fracture. Avoid hard, sticky, or chewy foods and try to chew on the opposite side until your permanent restoration is placed. Consistent brushing and flossing help maintain oral health and support the healing process.
Long-term success rests on restoring and protecting the tooth after the root canal. A well-designed crown or similar definitive restoration helps redistribute biting forces and seals the tooth against future contamination. With routine dental care and appropriate follow-up, an endodontically treated tooth can serve you reliably for many years.
Our team places a strong emphasis on comfort, clear instructions, and follow-up care to support a smooth recovery. If unusual symptoms appear after treatment — increasing pain, swelling, or persistent drainage — please contact us so we can assess healing and address any concerns.
Root canal therapy is a dependable way to relieve pain and save natural teeth when performed with careful diagnosis and skilled technique. If you’d like to learn more about root canal treatment at Chroma Dental or whether it’s the right option for you, please contact us for more information.
Root canal therapy is a dental procedure that removes infected or inflamed pulp from inside a tooth to relieve pain and stop the spread of infection. The treatment preserves the outer tooth structure while eliminating diseased tissue within the canal system. When successful, it restores comfort and allows the tooth to continue functioning in chewing and speaking.
At Chroma Dental we prioritize clear explanations, modern techniques and careful follow-up so patients know what to expect from diagnosis through restoration. Early assessment often lets clinicians treat problems before they become more complicated, making the procedure less invasive and more predictable. Your provider will review the reasons for treatment and the planned steps to protect long-term oral health.
Bacteria can reach the pulp through deep decay, cracks, chips or dental trauma, causing inflammation or death of the nerve tissue inside the tooth. Symptoms range from intense, throbbing pain and prolonged sensitivity to hot or cold, to swelling, drainage near the gum or a visible change in tooth color. Some infected teeth produce mild or no pain, which is why clinical examination and radiographs are important for accurate diagnosis.
If you notice ongoing pain, biting discomfort, lingering temperature sensitivity, localized swelling or a persistent gum bump, seek evaluation promptly. Early diagnosis preserves treatment choices and tends to make procedures simpler with better outcomes. Your clinician will combine your symptoms, exam findings and imaging to determine whether root canal therapy is indicated.
Modern non-surgical root canal treatment is performed under local anesthesia and typically involves isolating the tooth, creating a small access point, and using magnification and specialized instruments to clean and shape the canals. Clinicians use proven irrigation solutions and techniques to disinfect the canal system thoroughly before filling it with a biocompatible sealing material. The goal is to eliminate bacteria, seal the space, and prevent reinfection.
Some teeth are treated in a single visit while others require staged care when infection or complex anatomy is present, and sedation options can be offered for anxious patients. After endodontic therapy, the tooth usually receives a definitive restoration such as a crown to restore strength and protect against fracture. Your dentist will explain the expected timeline and any temporary measures between appointments.
Root canal treatment is performed with local anesthesia and is designed to relieve the pain caused by an infected or inflamed pulp rather than increase it, so most patients report much less discomfort during the procedure itself than they experienced before treatment. Mild soreness or sensitivity around the treated tooth and gums is common for a few days as tissues settle, and over-the-counter pain relievers usually manage this discomfort. Clinicians can prescribe stronger pain medication or antibiotics when clinically necessary.
If you have dental anxiety, sedation options may be available to help you remain comfortable and relaxed during care. If pain increases after treatment, or if swelling or drainage persists, contact your dental team promptly so they can assess healing and address any issues. Timely follow-up care and protection of the treated tooth reduce the risk of complications.
Immediately after treatment, follow your clinician’s instructions for pain control and oral hygiene; gentle brushing and flossing keep the area clean while tissues heal. Avoid chewing on the treated tooth while a temporary filling is in place and refrain from hard, sticky or chewy foods that could fracture the tooth. Maintaining routine dental visits and good home care supports long-term success.
Once a permanent restoration is placed, continue to protect the tooth with proper brushing, flossing and periodic dental exams. Report any new or worsening symptoms, such as increased pain, swelling or drainage, so your dentist can evaluate the restoration and the underlying root canal. Long-term function depends on both the quality of the endodontic procedure and the durability of the final restoration.
Restoring a tooth after root canal therapy is important because treated teeth can become more brittle and are at higher risk of fracture without protection. A crown is the most common definitive restoration because it redistributes biting forces, seals the tooth against contamination and replaces lost structure for long-term durability. The decision about restoration type depends on how much tooth structure remains and the tooth’s location and function.
Your dentist will evaluate the tooth and recommend the restoration that best preserves function and appearance while minimizing future problems. In some cases a post and core build-up or an onlay may be appropriate when enough structure remains. Timely placement of the final restoration is a key factor in long-term success after endodontic treatment.
When the pulp is irreversibly damaged, the main alternatives are extraction of the tooth or, in certain situations, monitoring if the tooth is asymptomatic and the patient prefers a conservative approach. Extraction eliminates the source of infection but introduces other restorative considerations, such as bridges, implants or removable appliances, to replace the missing tooth and preserve function. The best option depends on factors like the tooth’s restorability, surrounding bone, occlusion and the patient’s overall dental plan.
Your dental team will discuss the pros and cons of saving the tooth versus extraction, including long-term oral health implications and procedural complexity. Preserving a natural tooth when feasible often maintains bone and normal chewing patterns, but there are valid cases where removal and replacement are the prudent choice. A personalized evaluation helps determine a treatment plan that balances durability, function and patient preferences.
The lifespan of a root canal-treated tooth varies, but with proper restoration and oral hygiene many treated teeth function for decades and can last a lifetime. Success depends on thorough disinfection at the time of treatment, high-quality sealing of the canals, and placement of a durable final restoration to protect the tooth from fracture and reinfection. Regular dental checkups allow your provider to monitor the treated tooth and address problems early.
Factors that influence longevity include the tooth’s location, remaining tooth structure, bite forces, and individual health considerations such as periodontal status. Avoiding habits that stress teeth, like chewing hard objects, and addressing new dental issues promptly help maximize the long-term function of endodontically treated teeth. If concerns arise, your dentist can recommend options to reinforce or retreat a tooth when appropriate.
Although root canal treatment has a high success rate, failure can occur when bacteria persist or re-enter the canal system, when complex anatomy is missed, or when the final restoration does not adequately seal the tooth. Signs of failure include recurring or increasing pain, swelling, persistent drainage, a new gum bump near the treated tooth, or radiographic evidence of continued infection. Sometimes symptoms develop months or years after treatment, which is why ongoing monitoring is important.
If retreatment or endodontic surgery is indicated, your dentist or an endodontist will evaluate the tooth and discuss the options to resolve the problem while attempting to save the tooth. Prompt attention to warning signs improves the chances of successful retreatment. Your dental team will explain the recommended approach based on clinical findings and imaging.
Choose a provider who communicates clearly, explains diagnostic findings and walks you through the treatment steps, follow-up and restoration plan. Look for clinicians who use modern technology such as magnification, digital radiography and effective irrigation protocols to enhance precision and predictability. A practice that prioritizes patient comfort, offers sedation options when appropriate, and coordinates restoration after treatment supports better outcomes.
Discuss experience with endodontic procedures and ask how the office handles follow-up and complications so you understand the care pathway. A collaborative approach between your general dentist and an endodontist when needed can ensure complex cases receive the specialized attention they require. Clear expectations and coordinated restorative planning help protect your long-term oral health.
