Fear of the dentist is common — more people avoid care because of anxiety than most assume. If nervousness about noise, discomfort, or losing control keeps you from important dental work, the office of Chroma Dental provides carefully managed sedation options to make appointments calm, efficient, and predictable. Our goal is to remove anxiety as a barrier so patients can pursue lasting oral health with confidence.
Sedation dentistry is about improving the patient experience, not cutting corners. When used responsibly and tailored to an individual’s medical history and the planned procedure, sedation helps patients remain relaxed and cooperative so clinicians can deliver thorough, high-quality care in a single visit when appropriate.
Below you’ll find a clear, practical guide to how sedation works, who may benefit, the common methods used in dental practice, and what you can expect before, during, and after treatment. The emphasis here is safety, predictability, and restoring access to care for people who previously avoided the dentist.
Sedation targets the body's stress response so appointments feel manageable rather than overwhelming. Depending on the technique, patients may experience a gentle sense of relaxation, reduced awareness of procedures, or a deeper, dreamlike state while still retaining basic responsiveness. This helps limit memory of the appointment and reduces the physical tension that can make dental work harder for both patient and provider.
It’s important to understand that sedation complements, rather than replaces, local anesthesia. Local numbing still controls pain at the treatment site; sedation addresses the emotional and sensory aspects of the visit — the sounds, smells, and anticipatory fear — so the mouth can be treated with minimal distress.
Modern sedation is also highly monitored. The clinical team observes breathing, oxygen levels, and heart rate during the appointment and can adjust medication levels as needed. With trained professionals overseeing the process, many patients find the experience smoother and are more likely to keep up with preventive visits after a positive sedation experience.
Sedation is often the solution for people who delay care because of anxiety or traumatic past experiences. When fear drives avoidance, oral health can decline; sedation opens a path for patients to get the treatment they need in a controlled, supportive environment.
Other situations that commonly call for sedation include a strong gag reflex, heightened sensitivity to touch or sound, or a low tolerance for dental instruments. What may be an inconvenience for some can feel unbearable to others. Sedation quiets reflexes and sensory overload, enabling the clinician to work more efficiently and the patient to remain comfortable.
Patients facing long or complex treatment plans — those requiring extended chair time or multiple procedures in a single session — also benefit from sedation. Consolidating treatment can reduce the number of visits and the cumulative stress of care for individuals who have difficulty returning frequently.
Sedation is additionally helpful for people with special needs or certain medical conditions where a calm, controlled visit reduces risk. Each case is evaluated individually to match the depth of sedation to both medical and emotional requirements.
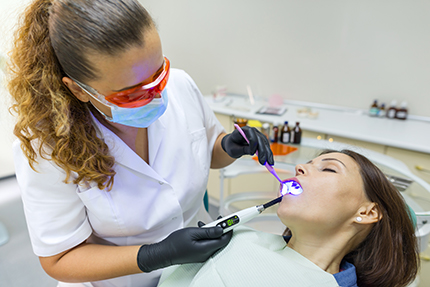
Determining the right sedation approach begins with a detailed review of medical history, current medications, allergies, and any previous reactions to sedatives or anesthetics. The planned procedures are considered as well — their length, complexity, and urgency all influence the choice. This pre-treatment evaluation is essential to crafting a plan that balances comfort with safety.
For mild anxiety and short procedures, inhaled nitrous oxide is often sufficient. When anxiety is more pronounced or the appointment will be lengthy, oral or intravenous (IV) options may be recommended. The guiding principle is always to use the lowest effective level of sedation to meet the patient’s needs.
Throughout sedation, clinicians monitor vital signs and patient responsiveness. Equipment and training for airway management and emergency response are part of responsible sedation practice. Because individual responses to medication vary, continuous observation helps ensure a stable and comfortable experience from induction to recovery.
Conscious sedation lets patients breathe independently and respond to verbal cues while feeling deeply relaxed and less aware of the procedure. This category includes nitrous oxide, prescribed oral medications, and office-administered IV sedation. Recovery tends to be relatively quick, although some forms require an escort home and a short period of rest afterward.
General anesthesia, by contrast, brings about a controlled unconscious state and is typically administered in a hospital setting by an anesthesiologist. It’s reserved for cases where office-based sedation is not appropriate or when specific medical or procedural factors demand a higher level of monitoring and support.
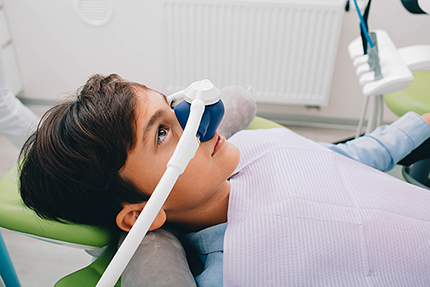
Inhaled nitrous oxide is a fast-acting option that produces mild to moderate relaxation and dissipates quickly after the gas is stopped. Because it is delivered with oxygen and titrated to the patient’s response, it’s a predictable, reversible choice for many shorter visits.
Good preparation helps ensure a predictable experience. Before any sedative is used, the team will review your medical history, medications, and any allergies. They will explain whether to take routine prescriptions on the day of treatment, provide guidance about eating and drinking, and confirm if an escort is required for your return home.
After the procedure, patients are monitored until it’s safe to leave. Depending on the method used, you may feel drowsy, have slowed reflexes, or experience mild short-term effects for several hours. Avoiding driving, alcohol, and heavy machinery for the remainder of the day is advised.
Your clinicians will provide clear post-operative instructions covering both the dental work itself and expected after-effects of sedation. They will outline signs that warrant prompt attention so you can resume regular activities confidently and know when to contact the office with concerns.
Safe sedation rests on careful patient selection, accurate dosing, continuous monitoring, and a team trained in emergency protocols. Adhering to established clinical standards ensures that relaxation never comes at the expense of safety. That framework provides peace of mind for patients and allows clinicians to focus on delivering precise dental care.
The experience and training of the care team directly affect the quality of the sedation experience. Competence in airway management, familiarity with monitoring equipment, and rehearsal of emergency responses are foundational elements of responsible office-based sedation.
If you’re wondering whether sedation could help you receive the dental care you need, a thoughtful conversation with your dental provider is the best next step. Discussing medical history, treatment goals, and personal concerns allows the team to recommend the most appropriate, evidence-based approach for your situation.
In short, sedation dentistry helps remove anxiety and sensory barriers so patients can access necessary treatment with safety and dignity. If nervousness, sensitivity, gagging, or the prospect of lengthy procedures has kept you from care, consider speaking with our team about personalized sedation options. Contact us for more information about how sedation can make your next dental visit easier and more comfortable.
Sedation dentistry uses medication to reduce anxiety and increase comfort during dental treatment by targeting the body's stress response. It complements local anesthesia, which controls pain at the treatment site, while sedation minimizes sensory stimuli and emotional distress so clinicians can work more effectively. The goal is a safe, calm visit that allows patients to receive needed care they might otherwise avoid.
The level of sedation ranges from minimal relaxation to deeper states where memory of the procedure may be reduced, and the choice depends on the patient's needs and the planned treatment. Throughout the appointment, trained clinicians monitor breathing, oxygen levels, and heart rate so medication levels can be adjusted as needed. This monitoring and professional oversight help maintain safety and predictability during sedation.
Patients who experience dental anxiety, have a strong gag reflex, or are overly sensitive to touch, sound, or smell commonly benefit from sedation. Sedation is also appropriate for people who require lengthy or complex procedures and prefer to consolidate care into fewer visits. Each patient is evaluated individually to match the sedation depth to medical history and emotional needs.
People with special healthcare needs or certain conditions that make cooperation difficult can also be candidates when office-based sedation is appropriate. The dental team reviews medications, allergies, and past responses to sedatives before recommending a plan. If a patient has significant medical concerns, coordination with a physician or consideration of hospital-based anesthesia may be advised.
Common office-based options include inhaled nitrous oxide, prescription oral sedatives, and intravenous (IV) sedation. Nitrous oxide acts quickly and wears off rapidly, making it useful for shorter visits and mild to moderate anxiety. Oral sedatives are taken before the appointment and provide deeper relaxation, while IV sedation offers precise control and rapid adjustment for longer or more complex procedures.
The choice of technique is based on the patient's medical history, the procedure's length and complexity, and the desired level of consciousness. Regardless of the method, local anesthesia is used for pain control at the treatment site. The dental team provides specific pre-treatment instructions and monitors the patient continuously to maintain safety.
Conscious sedation allows patients to breathe independently and respond to verbal cues while feeling relaxed and often less aware of the procedure. It includes nitrous oxide, oral sedatives, and many office-administered IV sedation techniques, and it usually permits a quicker recovery than deeper forms of anesthesia. Because the patient remains partially responsive, conscious sedation is appropriate for many outpatient dental procedures performed in the office.
General anesthesia produces a controlled unconscious state and is typically managed by an anesthesiologist in a hospital or surgical center setting. It is reserved for cases where higher levels of monitoring and airway control are required or when medical and procedural factors make office-based sedation unsuitable. A thorough assessment determines the safest environment for the required level of anesthesia.
Preparation starts with a detailed review of medical history, current medications, and any allergies or prior reactions to sedatives or anesthetics. The team will advise whether to take routine prescriptions on the day of treatment and will provide fasting instructions if IV sedation is planned. It is important to follow pre-appointment guidance exactly to reduce the risk of complications and ensure a smooth experience.
Patients who receive oral or IV sedation should arrange for a responsible adult to accompany them and drive them home after the visit, since reflexes and judgment can remain impaired for several hours. Wearing comfortable clothing and avoiding jewelry or contact lenses can also help during recovery. If you have questions about medications or specific health conditions, discuss them with the dental team before your appointment so the plan can be tailored to your needs.
During sedation, the dental team continuously monitors vital signs and responsiveness, adjusting medication as necessary to keep the patient comfortable and safe. Sensations vary by technique: nitrous oxide produces light relaxation, oral sedatives often result in drowsiness, and IV sedation can create a deeper, dreamlike state with limited memory of the procedure. Local anesthesia remains in place to control pain at the treatment site.
After the procedure, patients are observed until they meet recovery criteria and are stable for discharge. Common short-term effects include drowsiness, slowed reflexes, and temporary lightheadedness, so patients are advised not to drive, operate machinery, or make important decisions for the remainder of the day. The dental team will provide clear post-operative instructions and a contact number for any concerns during recovery.
Most side effects from dental sedation are mild and temporary, such as nausea, dizziness, or prolonged drowsiness, particularly with oral medications. More serious complications are uncommon but can include respiratory depression or adverse reactions to medications, which is why continuous monitoring and readiness for emergency response are essential components of safe sedation practice. Careful patient selection and appropriate dosing minimize these risks.
Patients with certain medical conditions or who take specific medications may face higher risks, so full disclosure of health history is critical before any sedative is used. The dental team is trained in airway management and emergency protocols, and equipment for monitoring oxygenation and heart rate is used during every sedated appointment. If you have concerns about risk, discuss them candidly with your provider so an informed plan can be made.
Many prescription and over-the-counter medications can interact with dental sedatives, altering their effectiveness or increasing side effects. Drugs that affect the central nervous system, certain antidepressants, blood thinners, and herbal supplements are examples that may require adjustment or additional precautions. A complete medication list helps the dental team select safe sedative options and dosing strategies.
In some cases, your provider may consult with your primary care physician or specialist to coordinate care and determine whether temporary medication changes are appropriate. Never stop prescribed medications without medical advice, and be sure to disclose supplements and recreational substance use. Transparent communication supports both safety and the best possible sedation outcome.
Children can receive sedation dentistry when appropriate, but their care requires specialized dosing, careful monitoring, and clear communication with parents or guardians. Nitrous oxide is commonly used for mild to moderate anxiety because it is easy to titrate and wears off quickly, while oral or IV sedation may be considered for more involved procedures or when a child cannot cooperate. The dental team will assess developmental status, medical history, and behavioral factors when recommending sedation for pediatric patients.
Consent from a parent or legal guardian is required, and arrangements for post-procedure supervision are essential because children may experience lingering drowsiness. Pediatric sedation may sometimes involve collaboration with a pediatric anesthesiologist for deeper levels of anesthesia or for children with complex medical needs. The focus is always on safety, appropriate dosing, and minimizing distress for the child.
If you are considering sedation dentistry, request a consultation so the team can review your medical history, discuss sedation options, and develop a personalized plan that matches your needs and comfort level. A consultation allows the clinicians to explain the risks and benefits, provide pre-appointment instructions, and answer specific questions about recovery and monitoring. This conversation is the best way to determine whether office-based sedation is the right choice for your care.
Chroma Dental serves patients in Midtown East and can provide guidance tailored to individual health considerations and treatment goals. To schedule an appointment or ask for more information, contact the office at (646) 419-8726 for new patients or (646) 440-3101 for existing patients, and consider reviewing your current medications and medical records beforehand to facilitate a thorough evaluation.
