Missing teeth affect more than appearance — they influence how you bite, speak, and how your facial structure ages. Modern implant dentistry rebuilds the tooth from root to crown, delivering a long-term solution that prioritizes function and natural appearance. By focusing on the underlying support rather than just the visible tooth, implant therapy helps patients regain the comfort and confidence of a stable bite.
Implants are engineered to act like natural tooth roots, providing a secure anchor for crowns, bridges, or dentures. This foundation supports predictable chewing and clearer speech while reducing the need to alter adjacent healthy teeth. For many people, the stability and durability of implants make them the preferred option over removable appliances.
We pair careful diagnostics with patient-centered planning to outline implant pathways that reflect each person’s oral health and lifestyle goals. At Chroma Dental, our approach emphasizes clear explanations, conservative surgical techniques, and restorative designs that blend seamlessly with your existing teeth.

One of the key advantages of an implant is its ability to maintain bone where a tooth once stimulated the jaw. When a tooth is lost, the surrounding bone tends to resorb over time; an implant replaces that stimulation and helps preserve bone volume. This preservation supports the soft tissues, helping to maintain a youthful jawline and natural facial contours.
Preserving bone also contributes to better long-term outcomes for adjacent teeth and restorations. By maintaining the ridge height and width, implants often simplify future restorative options and reduce the chance of needing more extensive corrective procedures.
Because implants function like natural roots, they also distribute chewing forces in a way that protects other teeth. This balanced force distribution improves comfort during everyday activities such as eating and speaking, and supports overall oral health.
Dental implants are biocompatible posts — generally made from titanium or titanium alloys — designed to integrate with the jawbone. The biological process of osseointegration describes how bone grows closely around the implant, creating a secure and lasting connection that supports a prosthetic tooth.
After an implant integrates, a restorative component (an abutment and crown, a bridge, or an overdenture) is attached to recreate the visible tooth structure. Contemporary implant systems offer a range of restorative materials and abutment options so clinicians can match color, contour, and bite dynamics for a natural result.
Long-term success is the product of precise surgical placement, digitally informed planning tools when indicated, and a restorative design that respects your bite and oral environment. Regular maintenance and good oral hygiene further protect the investment in your oral health.
Planning often begins with a thorough exam and digital imaging to visualize bone anatomy and nearby structures. Surgical guides or computer-assisted plans can help ensure implants are positioned to support predictable form and function. This preparation is essential for predictable esthetic and mechanical outcomes.
Surgical placement is commonly performed in an outpatient setting under local anesthesia; sedation options are available for added comfort. Depending on the technique and clinical needs, a temporary restoration may be placed immediately, or the site may be allowed to heal before fitting the final prosthesis.
Once the implant has integrated with the bone, the restorative team fabricates custom prosthetics that match your bite and smile. Follow-up care focuses on monitoring tissue health, controlling plaque, and maintaining routine professional visits to support longevity.
Implants improve more than appearance — they restore practical function. With a stable anchor in the jaw, implant-supported teeth let people eat a wider variety of foods, speak without concern for shifting restorations, and enjoy the confidence that comes from a reliable smile.
Because implants stimulate bone, they help slow the bone loss that can follow tooth extraction. This preservation supports facial structure and can reduce the risk of future restorative complications related to ridge collapse or loss of vertical dimension.
With disciplined oral hygiene and routine dental care, many implant restorations remain functional for years. Implants do not decay like natural teeth, and unlike traditional bridges, they usually allow adjacent natural teeth to remain untouched.
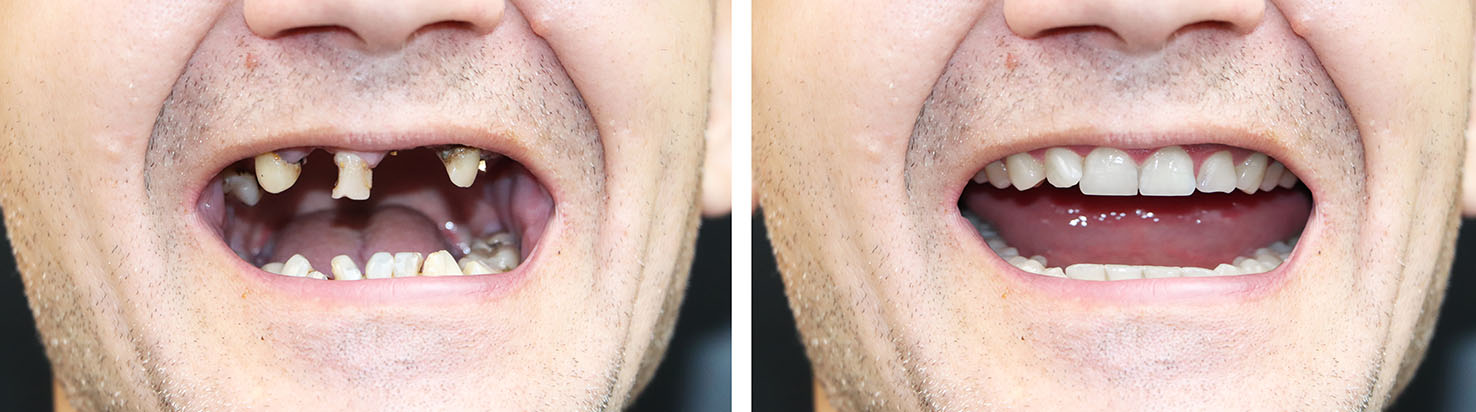
When one tooth is missing, a single implant restored with a crown offers a conservative replacement that leaves neighboring teeth intact. This approach maintains more of your natural dentition and provides a natural-feeling result that integrates with your bite and smile.
For several missing teeth in a row, implants can support a bridge so that healthy adjacent teeth aren’t used as anchor points. Strategically placed implants bear the load of the prosthesis and help preserve bone in the edentulous span.
Patients who are missing many or all teeth may benefit from full-arch implant restorations, which can be fixed or removable depending on goals. These solutions restore chewing efficiency and facial support and often allow for provisional teeth soon after surgery, with definitive restorations placed after integration.
Implants can also be used to secure removable prostheses, providing significantly improved retention and comfort compared with traditional dentures. Overdentures offer a practical middle ground that enhances function while remaining removable for hygiene and adjustments.
Candidacy depends on overall health, oral hygiene, bone volume, and treatment goals. Many patients are suitable candidates, and where bone is limited, techniques such as grafting, ridge expansion, or angled implant placement can expand options. A careful diagnostic process, including clinical exams and imaging, helps identify the safest, most effective path forward.
Treatment typically begins with a comprehensive evaluation and imaging to map anatomy and plan implant positions. Surgery is usually outpatient, and healing varies with individual biology and the complexity of the case. After osseointegration is confirmed, the restorative team creates custom prosthetics to match your bite, tone, and facial balance.
Follow-up focuses on hygiene instruction, periodic monitoring, and professional maintenance to protect the health of surrounding tissues and the integrity of the restoration.
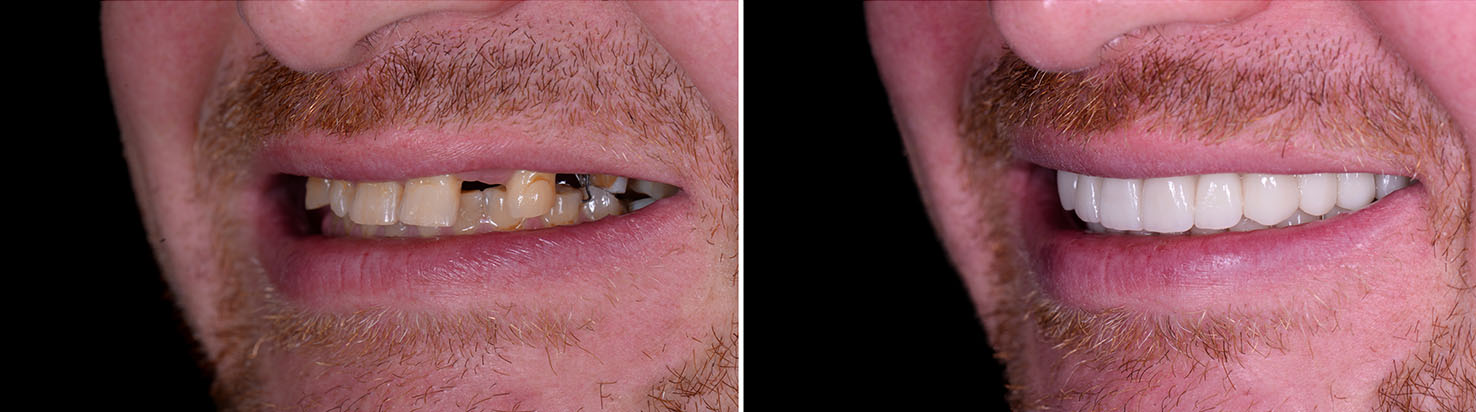
Bone grafting is often used when the jaw lacks sufficient volume to support implants. Grafting rebuilds the ridge to provide a stable foundation and better soft-tissue support, which can improve both function and esthetic outcomes. The choice of graft material and timing are tailored to each patient’s anatomy and treatment plan.
Performing grafting before or at the time of implant placement can increase success rates and enhance long-term stability. Our preference is to use minimally invasive techniques and evidence-based materials to achieve consistent, predictable outcomes.
Daily oral hygiene and routine dental visits are essential to protect implants and surrounding tissues. Professional cleanings and periodic assessments help identify and address soft-tissue inflammation or mechanical issues early, keeping restorations functional and comfortable for years.
Implant maintenance typically includes specialized cleaning techniques and education on tools that support tissue health. With attentive care, implants can remain a reliable part of your oral health plan.
Implant dentistry offers robust options for restoring missing teeth with solutions that prioritize function, appearance, and long-term oral health. Whether you’re exploring a single-tooth replacement or a more comprehensive restoration, careful planning and experienced execution are key to successful outcomes.
If you would like to learn whether implant therapy is appropriate for you, please contact us for more information. Our team can walk you through the process and help you make an informed decision about your care at Chroma Dental.
Dental implants are biocompatible posts, most often made from titanium or titanium alloys, that are placed in the jaw to replace missing tooth roots. Through a process called osseointegration, surrounding bone grows closely around the implant, forming a stable foundation for a prosthetic tooth. This integration allows the implant to support crowns, bridges, or overdentures with long-term mechanical stability.
Once the implant has integrated, a restorative component such as an abutment and crown is attached to recreate the visible tooth structure and bite relationships. Modern implant systems offer a range of restorative materials and abutment designs to match color, contour, and occlusion. Careful planning and precise placement are essential to achieve both functional and natural-looking results.
Good candidates for dental implants generally have missing teeth, adequate oral hygiene habits, and overall health that supports healing. Controlled chronic conditions such as well-managed diabetes typically do not preclude implants, but active infections, untreated periodontal disease, or certain systemic conditions may require evaluation and coordination with a physician. Bone volume and quality are important considerations, and patients with insufficient bone may be candidates after grafting or alternative planning.
A candidacy assessment includes a clinical exam, digital imaging, and a review of medical history to develop an individualized plan. Lifestyle factors such as smoking and bruxism are discussed because they can affect healing and long-term success. Your provider will explain options and any preparatory treatments needed to maximize predictability and comfort.
Treatment typically begins with a comprehensive consultation that includes digital imaging to map bone anatomy and adjacent structures, followed by a personalized surgical and restorative plan. Implant placement is usually performed in an outpatient setting with local anesthesia and optional sedation for comfort, and surgical guides or computer-assisted plans may be used to enhance precision. Depending on the clinical approach, a temporary restoration can sometimes be provided immediately or the site may heal before final restoration.
The biological integration phase varies by individual and by the specifics of the case, with follow-up appointments to monitor healing and tissue health. After osseointegration is confirmed, the restorative team fabricates and fits a custom prosthesis designed to match your bite and esthetics. Routine maintenance and periodic professional visits are scheduled to protect the investment and ensure long-term function.
Implants restore a missing tooth root, which helps preserve bone and maintain facial contours, whereas traditional bridges rely on adjacent teeth for support and removable dentures rest on the soft tissues. Because implants do not typically require alteration of neighboring healthy teeth, they can be a more conservative long-term option for single-tooth replacement. Implant-supported restorations also distribute chewing forces through the jawbone, improving comfort and function compared with many removable options.
Removable dentures can be appropriate for some patients and offer non-surgical solutions, but they may feel less stable and require ongoing adjustments. Implant-supported overdentures or fixed prostheses address many of the functional limitations of conventional dentures by improving retention and chewing efficiency. Treatment selection is individualized based on oral health, anatomy, patient preferences, and clinical goals.
Bone grafting or sinus augmentation is considered when the jaw lacks sufficient height or width to support predictable implant placement. Tooth loss, long-standing extractions, or anatomic variations can lead to ridge resorption, and grafting rebuilds the foundation to achieve better implant stability and soft-tissue support. The choice of graft material and timing are tailored to the patient's anatomy, healing potential, and the planned restoration.
Grafting can be performed as a staged procedure before implant placement or at the time of implant surgery in select cases, depending on the clinical needs. These procedures are commonly used to expand treatment options and improve long-term outcomes by creating a more favorable environment for osseointegration. Your clinician will explain the benefits, expected healing timeline, and any alternatives during the planning phase.
Implants can support a wide range of restorations, from single crowns that replace one missing tooth to implant-supported bridges that span several adjacent missing teeth. For patients missing a full arch, implants can anchor fixed full-arch prostheses or removable implant-retained overdentures, providing restored function and facial support. The restorative choice depends on the number of missing teeth, bone availability, esthetic goals, and patient preferences.
Prosthetic components and materials are selected to match tooth shade, contour, and bite dynamics, and digital workflows often enhance fit and esthetics. In many cases, provisional restorations are used during healing to maintain appearance and function while integration occurs. Final restorations are designed to balance comfort, chewing efficiency, and long-term maintenance.
Long-term implant success relies on disciplined daily oral hygiene that includes effective brushing and cleaning around implant restorations, along with interdental cleaning using floss, interdental brushes, or water irrigation where appropriate. Avoiding harmful habits such as smoking and refraining from using teeth as tools helps protect implants and surrounding tissues. Home care routines should be discussed and individualized with your dental team to address prosthetic design and tissue contours.
Regular professional maintenance appointments are essential and typically include removal of biofilm and assessment of tissue health to detect early signs of inflammation or mechanical issues. Specialized cleaning techniques and instruments may be used to safely maintain the implant surface and soft tissues. At Chroma Dental, our team provides tailored maintenance instruction and schedules periodic reviews to preserve implant health over time.
As with any surgical procedure, implant placement carries risks such as infection, swelling, bleeding, and temporary or, rarely, lasting nerve or sinus complications if nearby anatomy is affected. Careful preoperative assessment, precise surgical technique, and adherence to postoperative instructions help minimize these risks. Early recognition and management of complications are important to protect osseointegration and overall outcomes.
Longer-term complications can include peri-implant mucositis and peri-implantitis, which are inflammatory conditions that affect the soft tissues and supporting bone around implants. These conditions are influenced by oral hygiene, systemic health, and smoking, and they underscore the importance of maintenance and timely professional care. If concerns arise, your clinician will recommend appropriate treatments to control inflammation and preserve the restoration.
Advanced imaging such as cone beam computed tomography (CBCT) allows clinicians to evaluate three-dimensional bone anatomy, vital structures, and spatial relationships before surgery, improving diagnostic accuracy and safety. Digital planning tools and surgical guides translate virtual plans into precise clinical placement, reducing variability and enhancing prosthetic-driven positioning. These technologies support more predictable esthetic and functional results while helping clinicians anticipate and address anatomic challenges.
Digital impressions, CAD/CAM design, and milled or 3D-printed prosthetics contribute to improved fit, occlusion, and efficiency in fabrication and delivery. When combined with conservative surgical techniques, these tools streamline the process and often reduce chair time and adjustments during restoration. The office of Chroma Dental incorporates digital workflows when indicated to enhance planning precision and patient comfort.
Recovery after implant surgery commonly includes mild to moderate discomfort, swelling, and minor bruising during the first few days, which are managed with prescribed or over-the-counter medications and cold therapy as advised. Patients are typically given clear postoperative instructions regarding oral hygiene, diet, and activity levels to support healing and minimize complications. Most people return to normal activities within a few days, though healing and integration continue over several weeks to months depending on the case.
Dietary modifications such as soft foods and avoiding chewing directly on the surgical site are recommended during initial healing, and follow-up visits ensure the tissues are progressing as expected. Patients should contact the dental office for persistent pain, excessive swelling, fever, or any signs of infection so the care team can intervene promptly. Routine checkups and professional maintenance support long-term comfort and function after recovery.
